Objectives
The acute respiratory distress syndrome (ARDS) is a serious disease secondary to lung injury , causing edema and a severe lung inflammation, hypoxia , and an activation of cellular coagulation. Mechanical ventilation with positive end-expiratory pressure (PEEP) is the first-line of treatment to maintain gas exchange that is compatible with survival. However, inappropriate ventilator settings can generate lesions induced by mechanical ventilation (LIMV) and are responsible for excess mortality. While there are compelling arguments for the use of small tidal (VT) volumes in ARDS, the level of PEEP applied remains controversial. Prone ventilation (PV) is also frequently used to improve oxygenation without the pathophysiology of its effects being perfectly known. Finally, the constant high mortality of ARDS (about 50%) justifies experimental and clinical research in an attempt to improve the prognosis.
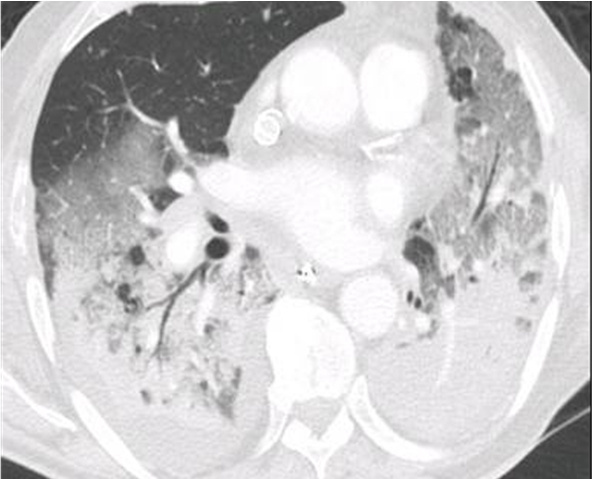
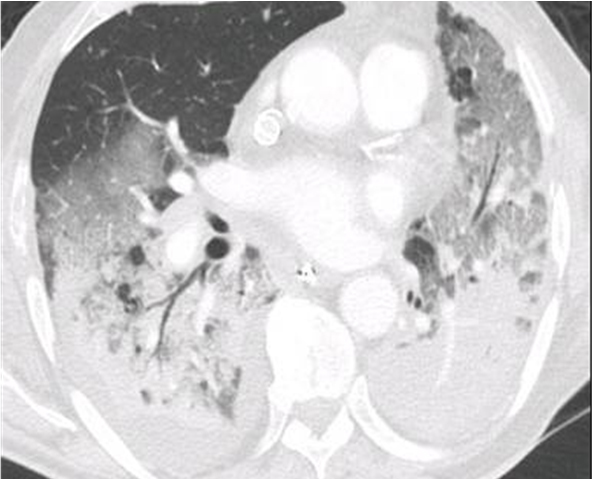
Pulmonary imaging allows us to obtain regional information on lung physiology in a noninvasively manner. Its contribution was fundamental in the study of ARDS where the pulmonary lesions are very heterogeneous (Figure 1), and therefore misinterpreted by conventional survey tools (blood gas, respiratory mechanics...). The thoracic scanner has led to major advances in understanding the pathophysiology mechanisms involved in ARDS and of the effects of ventilator treatment of this disease (PEEP, PV...). However, the relatively important radiation of this exam, and the need to use non-physiological tracer (iodinated contrast agents, xenon...) limit the extension of the application of this method to the study of other physiological phenomena.
The objectives of the research team are:
1. Evaluate the pathophysiological mechanisms of lung injury and determinants of LIMV on animal tests.
2. Evaluate new pharmacological and ventilator therapies for ARDS and LIMV on animal tests.
3. Describe on humans patients the regional distribution and evolution of pulmonary physiological disturbances occurring during ARDS, to better understand the effects of mechanical ventilation on lung parenchyma to minimize the deleterious effects.
4. Evaluate new therapeutic strategies in humans using imaging modalities.
Our team has developed functional imaging tools applied to the study of this problem, in the context of their application in patients with ARDS. Positron emission tomography (PET) was originally chosen as a preferred method of study. This exam provides invaluable information for the study of the problem since it is the only imaging method that measures reliably and noninvasive perfusion, ventilation and pulmonary inflammation in a combined manner. Furthermore, these three parameters are central to the pathophysiology of ARDS, but also to that of LIMV. The main limitation of this imaging modality is the need to transport critically ill patients to the PET scanner, which can be problematic in unstable patients. For this reason, alternative imaging techniques potentially useful at patient bedside were evaluated in a second time.
The research topics have been broken down into four areas:
1. Validation of PET for measuring physiological pulmonary parameters on animal tests.
2. Application of PET to the study of ventilator and pharmacological treatment of ARDS on animal tests.
3. Validation of the alternative imaging techniques that may be used at patient bedside.
4. Clinical research.
Figure 1. Thoracic scanner image of a patient suffering from ARDS
Research axes